Chronic pelvic pain
About chronic pelvic pain conditions
Pain in and around the pelvis which lasts more than 6 months is referred to as chronic pelvic pain. This condition can affect 1 in 6 women and can be very disruptive and distressing.
What causes the pain?
There are many possible causes of pelvic pain and it can be a combination of physical and psychological components.
Conditions which can cause chronic pelvic pain, include:
- Endometriosis – cells of the lining of the womb (endometrium) are found elsewhere in the body, usually the pelvis
- Adenomyosis – the lining of the womb (endometrium) is found in the muscle of the womb which can cause pain around the time of a period and during sex
- Pelvic inflammatory disease – infection in the fallopian tubes and/or pelvis
- Interstitial cystitis (also known as bladder pain syndrome) – bladder inflammation
- Previous surgery in and around the pelvis
Sometimes, there may not be a physical condition linked to chronic pelvic pain. There could be a problem with the perception of pain by nerve endings in the pelvis (neuropathic pain). Alternatively, some mental health conditions can also contribute to an increase in the sensitivity of pain.
Pelvic floor relaxation
An important stage in improving many symptoms is recognising when the pelvic floor muscles are tight, knowing how to enable them to release and to acknowledge when they are relaxed.
Like other muscle groups in the body, the pelvic floor muscle has a scale of activity. When we contract, or tighten the pelvic floor, it should lift and when we let go of the contraction, the muscles should return to their resting position. When muscles are not able to let go, this can also lead to pain and further consequences which may affect the bladder or bowel.
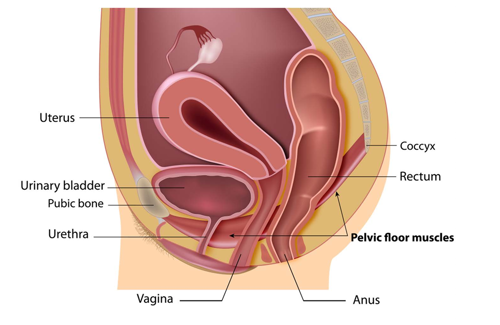
The pelvic floor muscles form a hammock underneath your pelvis to provide support and control for your bladder and bowel. The muscles attach to your pubic bone at the front, then span backwards to your coccyx (tailbone) and outwards to your sitting bones.
How to perform a pelvic floor contraction
A pelvic floor contraction is performed by closing and drawing up your front and back passages. Imagine you are trying to stop wind and at the same time trying to stop your flow of urine. It should be a sensation of ‘tighten and lift’.
You should:
- Continue to breathe normally
- Keep your buttocks and legs relaxed though you may feel a gentle tightening of your tummy
- Always let the muscles fully relax at the end of a contraction
Getting to know how it feels to contract the muscles is an important step in knowing when they are working, as well as when they are relaxed. It is easiest to practise this in a sitting or lying position.
When you understand how to contract and relax them, there are other exercises which can be useful to achieve relaxation.
Lift and let it go in stages
During this exercise, imagine the pelvic floor is a lift in a 3-storey building. Contract the pelvic floor muscles a little to lift to the first floor, pull in a little bit more to go to the second floor, squeeze a little more to go to the top. Continue to gently breathe throughout each hold.
Now slowly allow the muscles to release to go down to the second floor, release a little more to go to the first floor, let the muscle relax further back to the ground floor, and now let them fully release down to the basement.
Allow the pelvic floor muscles to soften, widen and lengthen – there is no need to push or bear down.
Let them soften, lengthen, and melt. This takes practice to achieve, and you may start with less stages and progress.
Management options
There are a variety of treatment options that can be tried. The response varies between individuals, so it is worth trying different things to see which will help you and often it is a combination that seems to be useful.
Pelvic floor relaxation exercises
The following exercises can assist with pelvic floor relaxation. Aim to hold each position for 30 to 60 seconds and repeat 2 to 3 times.
To start with, you may benefit from completing these exercises little and often to promote pelvic floor relaxation. Over time you may add these into your normal exercise/stretching/yoga routines.
Need more help?
Consider self referring using the link below:
If you have a new injury or problem, please look at the self help information in our advice pages. We will often complete the same exercises and share information in clinic appointments.
If you still need some more help you can self refer into our service. Please note that the NHS is currently experiencing longer than normal waits, for more information visit our waiting times page.










